Personalised Stratified Follow-Up: Guidance to accelerate implementation in response to COVID-19
1. Download Original Documents
- PDF of the guidance (Jan 21 v1.1)
- Excel of Appendix 1 – the checklist (v1.1)
- Word doc of Appendix 2 – the resources (v1.1)
2. Purpose
This document is a COVID-19 recovery planning resource to assist MDTs and Trusts to support changes to follow-up for all patients with cancer, after initial treatment is completed. It outlines:
- guidance on accelerating implementation across all cancers
- the principles of Personalised Stratified Follow-Up (PSFU), which includes the delivery of personalised cancer care interventions for all patients
- a checklist to help mitigate the risk of patients being lost to follow-up during COVID-19 surges.
- a suite of resources to support implementation
This document should be read in conjunction with:
- NHS England/Improvement’s Handbook for implementing Personalised Stratified Follow up in cancer (2020)
- NHS England/Improvement & NHSX’s Digital Remote Monitoring Follow Up Guide (2021)
- NHS England/Improvement’s guidance on Implementing Phase 3 of the NHS response to the COVID-19 pandemic (2020), specifically Section 4 on Patient Initiated Follow Up.
This document should be read in conjunction with:
- NHS England/Improvement’s Handbook for implementing Personalised Stratified Follow up in cancer (2020)
- NHS England/Improvement’s guidance on Implementing Phase 3 of the NHS response to the COVID-19 pandemic (2020), specifically
3. Background
What is personalised care?
Personalised care represents a new relationship between people, professionals and the system. It happens when we make the most of the expertise, capacity and potential of people, families and communities. Personalised care is based on ‘what matters’ to people and their individual strengths and needs. It also takes into account the people that they care for and those that may care for them.
Personalised care gives people the same choice and control over their mental and physical health that they have come to expect in every other aspect of their life. A one-size-fits-all health and care system simply cannot meet the increasing complexity of people’s needs and expectations.
Personalised care in cancer includes a range of interventions that all cancer patients should have. These interventions are:
- Shared decision making about treatment and follow up options
- Personalised care and support planning (including holistic needs assessments) at the time of diagnosis, at the end of treatment, and at times in between where there are significant changes (physical, emotional/psychological and social) for the patient
- Treatment summaries provided to the patient and their primary care team at the end of a phase of treatment
- Health & wellbeing information and support
- Holistic cancer care reviews and long term management in primary care
What is personalised stratified follow up?
A model of follow-up in which the clinical team and the person living with cancer make a decision about the best form of aftercare based on the individual’s clinical and personalised needs. Individuals enter either a professional led or a patient initiated follow up (PIFU) pathway.
- Professional Led Follow Up Pathway: The follow-up pathway in which individuals with cancer continue to have face to face, video, phone, or email contact with their clinical team as part of continuing follow up. Follow up may be led by doctors, nurses or specialist allied health professionals. Follow up may be delivered by the specialist team or by the primary care team.
- Patient Initiated Follow Up Pathway: The follow-up pathway in which patients are empowered with the knowledge and skills to self-manage their condition. They are given information about the symptoms to look out for and who to contact if they notice any of these alert symptoms, future scheduled tests, and how to contact the specialist team if they have any concerns. They do not receive any further outpatient appointments unless further investigations or support is required. PIFU may also be known as Open Access Follow Up (OAFU), Patient Triggered Remote Follow Up (PTFU) or Supported Self Management Follow Up (SSMFU).
As PSFU it is a core component of personalised care, PSFU should be introduced to the patient early in their cancer pathway. This is so that they are fully informed and understand the variety of ways in which they may be followed up after their initial treatment ends.
The diagram below from the National Cancer Survivorship Initiative (2013) shows the key interventions and support from services required on the PSFU pathway.
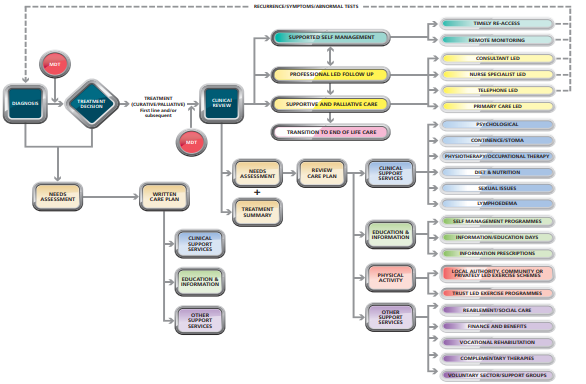
Guidance for implementing PSFU
Why do we need to accelerate implementation of PSFU?
In the current climate of COVID-19, personalising aftercare along the whole cancer pathway is more pertinent than ever. Whilst this has been mainly driven by capacity issues, individual risk assessment and patient choice to avoid clinical settings, the goal to provide personalised care is not new. When personalised care is provided sincerely, it is a fundamental way to prevent widening health inequalities and to reduce existing inequalities within our patient population.
NHS England/Improvement’s guidance on Implementing Phase 3 of the NHS response to the COVID-19 pandemic outline many benefits of PIFU specifically:
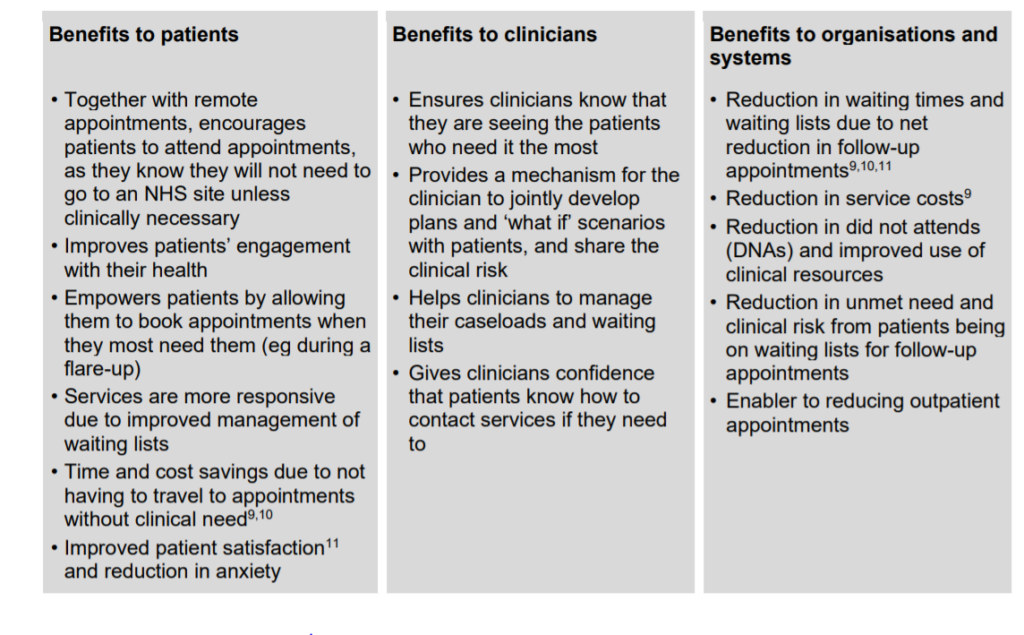
What are the key features of PSFU?
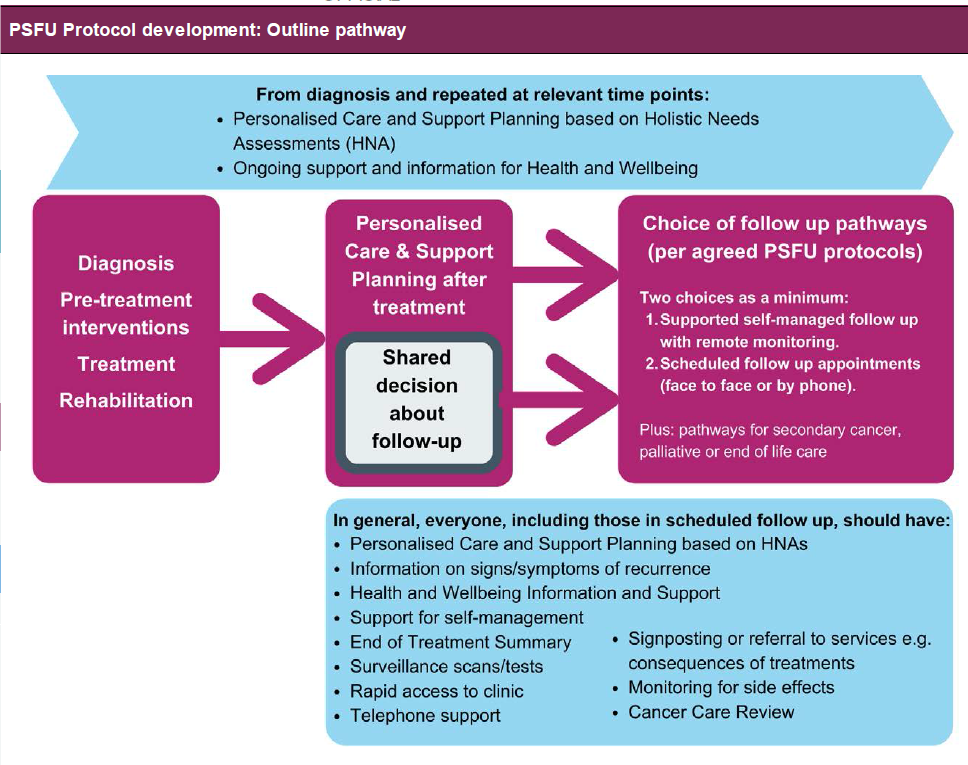
The National Cancer Survivorship Initiative (NCSI, 2013) advises that individuals are assessed early in the treatment pathway to determine which follow-up process would best meet their needs and identified the following key features:
- Effective needs assessment at the point of diagnosis and end of treatment that identifies and addresses any outstanding needs and ensures the patient has knowledge and confidence to self-manage.
- Removal of routine follow-up appointments from the pathway. The results will be reviewed by an appropriately qualified staff member and the patient is informed of the results (as per clinical judgement and local protocols).
- Good communication between specialist, community and primary care teams
- A robust remote monitoring system to manage on-going surveillance tests and ensure no one is lost to follow-up
- A system that allows rapid re-entry into the specialist cancer service as required. This reassures individuals that they are able to access appropriate, named support quickly should they need it, without having to go via their GP.

4. Principles to accelerate implementation of PSFU across all cancers
A great deal of work has already occurred across London to implement PSFU in breast, colorectal and prostate cancers. A self-assessment checklist has been developed for MDTs/Trusts to utilise as a resource to implement PSFU across additional cancer pathways and support safety netting processes for patient tracking list management (Appendix 1). This has been adapted from the East of England Cancer Alliance tool (2020). This document also includes a suite of resources relevant for London (Appendix 2).

Principle 1
Clinical leadership and resource is required to implement PSFU
Executive buy-in for PSFU is needed at both Trusts’ Cancer Board level and within Alliance recovery plans. At both levels, PSFU in cancer should be a shared objective between the Cancer Alliance’s cancer recovery plan and the STPs’ outpatient transformation programmes (and therefore embedded into STP/ICS Gold structures). By combining the governance with clinical leadership, it is expected this will lead to opportunities for resource and strategic focus.
An MDT clinical ‘sponsor’ should also be identified for implementing PSFU at tumour level. The sponsor will need to ensure the PSFU pathway is safe and pragmatic, including when it spans primary, secondary and tertiary services.
As governance and protocols will vary between tumour sites and between organisations, it is important that MDTs follow local clinical governance structure and protocols.
Resources:
- Personalised Stratified Follow-up handbook NHS England/Improvement Cancer Programme
- Early Breast Cancer SFU Implementation Resource Pack South East London Cancer Alliance
- PSFU Breast Cancer Clinical Guidelines RM Partners
- LCA Colorectal Cancer Clinical Guidelines RM Partners
- Colorectal Surveillance protocol RM Partners
- London Cancer Early Breast Cancer Stratified Follow–Up Implementation Resource Pack North Central and East London Cancer Alliances
- UCLH Cancer Collaborative Colorectal Stratified Follow up Implementation Resource Pack North Central and East London Cancer Alliances
- London Cancer Prostate Cancer Stratified Follow up Implementation Resource Pack North Central and East London Cancer Alliances
- Prostate Cancer SFU Implementation Resource Pack North Central and East Cancer Alliances
- Breast Cancer PSFU: SOP West Middlesex Hospital Trust
- Pan London personalised cancer care key performance indicatorsTransformation Partners in Health and Care
- Business planning and commissioning PSFU University of Southampton and Transformation Partners in Health and Care

Principle 2
Personalised care interventions are an integral part of cancer follow up
PSFU pathways must include all personalised cancer care interventions delivered by the hospital team – this includes shared decision making, Holistic Needs Assessment with a care plan; Treatment Summary; Health & Wellbeing information & support.
The personalised care principle of shared decision making should be used to determin which strata of follow up (i.e. professional led or PIFU) a patient is most likely to go on at the end of their initial treatment. This conversation should take place as early as possible in the patient’s treatment pathway, recognising that it may change.
Health and Wellbeing information & Support may be delivered jointly by NHS primary, community, acute teams, and with voluntary sector services. NHS England/Improvement has published a Health & Wellbeing Information & Support self-assessment checklist.
Patients should also be supported with a Cancer Care Review and long term management care plan by their primary care team. Separate guidance from London on managing cancer as a long term condition for COVID recovery has been published.
It is imperative for patients to receive all this information from the onset, in order to facilitate a clear understanding of the management of their condition. This ultimately promotes patient empowerment and reduces levels of anxiety and fear by knowing what to expect from their clinical teams, especially when this spans multiple services.
Resources:
- Health and Wellbeing Information & Support checklist NHS England/Improvement
- Electronic Holistic Needs Assessment Macmillan
- Treatment summaries: How To guide Macmillan
- Health and Wellbeing: How to Guide Macmillan
- Providing wellbeing activities during COVID-19 outbreak confinement period: Guidance and Video Macmillan
- Social prescribing guide for Primary Care Networks Macmillan
- Providing personalised care for people living with Cancer Macmillan
- Principles and tools for Cancer Care Reviews and managing cancer as a long term conditionTransformation Partners in Health and Care and Macmillan
- Comprehensive model of personalised care NHS England/Improvement

Principle 3
Virtual appointments are a core element of PSFU
Decisions to stratify patients should be made as early as possible in the treatment pathway, and with the ethos of shared decision making. Follow up regimes, both during treatment and after treatment ends, will usually be structured as follows:
• Professional led, face to face appointments
• Professional led, virtual appointments
• Patient initiated (PIFU), virtual appointments
For many reasons, clinicians and patients may also decide that a change in follow up regime is appropriate. Therefore there should be a mechanism for reviewing the shared decision, for example (but not limited to) changes in surveillance test results or a change in social circumstances. Consideration of which pathway the patient is on should be reviewed at every OPA/contact – especially if they are on a professional led pathway and can be moved to patient initiated follow up.
In the COVID-19 Phase 3 guidance, the NHS England/Improvement National Cancer Team has stipulated that cancer alliances should implement at least two additional PSFU pathways over and above breast, colorectal and prostate cancer pathways by 2023/24. Pan London clinical protocols with eligibility criteria will be developed for some tumour types through the pan London tumour working groups and STP Cancer GP Leads group, which in turn will be approved via NHS England’s cancer hub and Clinical Advisory Group. Trusts are advised to liaise with their Cancer Alliance regularly in order to confirm whether there are new clinical protocols in place. Trusts are also encouraged to utilise the PSFU principles and guidance to progress implementation where there is appetite to do so locally.
Resources:
- Video consultations for secondary care NHS England/Improvement
- COVID-19: guide for rapid implementation of remote consultations Chartered Society of Physiotherapy
- Principles of safe video consulting in general practice NHS England/Improvement
- Guidance on the introduction and use of video consultations during COVID-19: important lessons from qualitative research BMJ Journal
- Equality impact assessment of the NHS Long Term Plan (2019) specifies legal duties and requirements of the NHS to give due regard or regard to addressing health inequalities and advancing equality of opportunity NHS England/Improvement

Principle 4
Robust patient tracking and remote monitoring systems are integral to patient safety
All trusts need to ensure their remote monitoring system has the most up to date version and that any technical issues are regularly feedback to the IT provider.
London cancer alliances have an agreed specification for remote monitoring systems to facilitate robust tracking and safety netting of patients. Please see the resources for an example Project Initiation Document that includes essential and desirable criteria for remote monitoring systems.
Resource:
- NHS England/Improvement & NHSX: Digital Remote Monitoring System Follow Up Guide
- SFU Remote Monitoring IT system PID North Central East London Cancer Alliance
- SOMERSET RM System: guidance, website and email
- INFOFLEX RM System: Website and email
- Guidance for professionals on managing virtual consultations Macmillan
- Prostate Pathway SOP North Central & East London Cancer Alliances

Principle 5
Clear and timely communication between primary and secondary care teams is required for safety and good outcomes
It is imperative that acute teams communicate in a timely way with their primary care colleagues and vice versa.
The level of information provided to primary care should also be appropriate for primary care teams and patients. Treatment summaries are the preferred method of communicating the end of a patient’s phase of treatment.
Resources:
- GP information leaflet on supported self management North Central London Cancer Alliance
- Suite of top 10 tips for primary care professionals Macmillan

Principle 6
MDTs must provide end of treatment clinic appointments for all patients, to transfer patients to PSFU safely
An end of treatment appointment must include the following as a minimum:
- a post-treatment holistic needs assessment and refreshed care plan
- signposting to health & wellbeing information and support
- referrals to any health or social care services as required
- a treatment summary provided to the patient and their primary care team.
Treatment summaries should include the SNOMED codes that primary care teams will record on their clinical systems. This will facilitate primary care to safety netting for long term condition management. A summary list of codes is included in the resources section.
To further support safe transfer to PSFU, discussions on follow up regimes should be held with the patient as early as possible in the patient’s pathway. Other personalised care interventions, such as cancer care reviews and long term management in primary care, will also provide structure for the patient to support safe transfer to PSFU.
Resources:
- Treatment Summary Template National Cancer Survivorship Initiative
- UCLH Cancer Collaborative Electronic Safety Netting Toolkit for Cancer: The EMIS Web user guide North Central and East London Cancer Alliances
- Breast Cancer PSFU: SOP West Middlesex Hospital Trust

Principle 7
Re-access to specialist teams should be clearly defined for people with suspicion of a subsequent cancer
Patients and their carers need to be educated through health and wellbeing interventions to understand the red flags for referrals and referral routes, as addressed by previous patient education pathways.
Rapid access to secondary care advice and guidance should be easily available to primary care teams and other senior healthcare professionals. Primary care should safety net their patients when re-accessing oncology services for suspicion of subsequent cancers. MDT discussions should access the patient’s surveillance test results and these should be communicated to primary care in a timely way.
Hospital teams should consider that their re-access routes include:
• self-referral (PIFU)
• from primary care professionals (including GPs, senior General Practice Nurses, Pharmacists, Dentists)
• from allied health professionals (e.g. consultant physiotherapists, dieticians, occupational therapists and speech & language therapists).
Resources:
- Breast Cancer PSFU: SOP West Middlesex Hospital Trust

Principle 8
There should be clear routes to access services when symptoms/ conditions develop, related to the physical and psychosocial consequences of treatment
Rapid access to generalist and specialist advice and guidance on consequences of cancer and its treatment should be easily available to those clinically responsible for patients on PSFU pathways.
When patients present to primary care with signs or symptoms, they should also safety net their patients when requiring access to services for consequences of cancer and its treatments.
Primary care professionals are ideally placed to identify and initially respond to patient concerns with potential consequences of cancer treatment. When appropriately trained, primary care professionals will facilitate access to early diagnosis of the consequences of cancer and its treatment. Training needs assessments may be required to identify training gaps in primary care in terms of knowledge of cancer consequences of treatment.
Resources:
- SafeFit trial information Macmillan
- Consequences of Cancer Toolkit Royal College of GPs
- Commissioning Guidance for Lymphoedema Services for Adults Living with and Beyond Cancer TCST, Transformation Partners in Health and Care
- TCST Improving Psychologically informed cancer care: implementing the London Integrated Cancer Psychological Care Pathway and the development of Psycho-oncology services TCST, Transformation Partners in Health and Care
- Integrated Care System Guidance for Cancer Rehabilitation: A guide to reducing variation and improving outcomes in cancer rehabilitation in London TCST, Transformation Partners in Health and Care
- Allied health professionals’ role in rehabilitation during and after COVID-19 NHS England/Improvement

Principle 9
MDTs should use the self assessment checklist and audit to support implementation and embedding all aspects of PSFU pathways safely.
In addition to the checklist, MDTs will want to conduct clinical audits of patient cohorts on PSFU, for both safety and research purposes. If resourcing permits, begin auditing as soon as possible or alternatively undertake a short scoping exercise to complement any future audits.
Audits should examine changes to Personalised Care interventions throughout the treatment and follow up pathway, evaluating what changes can be modified to bring in line with models of Personalised Care Interventions, including PSFU.
An inequalities impact assessment should also be completed to ensure changes reduce existing inequalities in access and outcomes, and that they do not contribute to widening inequalities in these areas.
Resources:
- Suggested Audit tool to track PSFU discharges North Central London Cancer Alliance
- PSFU Audit Support Tool NHS England/Improvement
- Prostate PSFU Patient evaluation North Central and East London Cancer Alliances
- Coronavirus Hub Macmillan
- Patient leaflet for breast cancer West Middlesex Hospital
- Patient information leaflet sample North Central London Cancer Alliance
- Patient Information and video about accessing primary care and cancer care in general during Covid Kent and Medway CCG
- Cancer care map

Principle 10
MDTs should proactively assess patient experience and provide clarity on what is expected of patients and of the service.
Local guidelines and standardised operating procedures (SOPs) should be developed and followed, clearly outlining the patient information provided regarding:
• What patients and carers can expect throughout the PSFU pathway.
• What is expected of patients and carers throughout the PSFU pathway, for example going for tests, cancelling appointments etc
MDTs should routinely evaluate patient experience on the PSFU pathways. Data should be analysed to highlight any inequalities, support service improvements and contribute to research on patient outcomes.
Resources:
- Coronavirus hub Macmillan
- Patient leaflet for breast cancer West Middlesex Hospital
- Patient information leaflet sample North Central London Cancer Alliance
- Patient Information and video about accessing primary care and cancer care in general during Covid Kent and Medway CCG
- Cancer Care Map
- London Cancer Wellbeing London’s cancer alliances
5. Acknowledgement
This document has been drawn together from experts in personalised cancer care across London, representing the following cancer alliances:
- North Central London
- North East London
- South East London
- RM Partners (South West and North West London)
This document has been developed based on:
It has been led and coordinated by Transforming Cancer Services Team (TCST) for London, part of Transformation Partners in Health and Care through a COVID & PSFU working group.
With thanks to the following working group members who co-produced the document:
- Liz Price (chair), TCST
- Ana Agusti, NHS England/Improvement (London region)
- Vanessa Brown, RM Partners
- Sharon Cavanagh, North Central London Cancer Alliance
- Navneet Deol, Barts Health NHS Trust
- Diane Dunn, Imperial College Healthcare NHS Trust
- Sophie Lansdowne, South East London Cancer Alliance
- Matthew Miles, South East London Cancer Alliance
- Janice Minter, St George’s University Hospital NHS Foundation Trust
- Lisa Reid, The Princess Alexandra Hospital NHS Trust
- Karen Robb, North East London Cancer Alliance
- Emma Tingley, Macmillan Cancer Support (London region)
- Jason Tong. TCST
- Sam Tordesillas, South East London Cancer Alliance
- Alan White, RM Partners
- Melissa Wright, RM Partners
- Sarita Yaganti, North Central London Cancer Alliance
