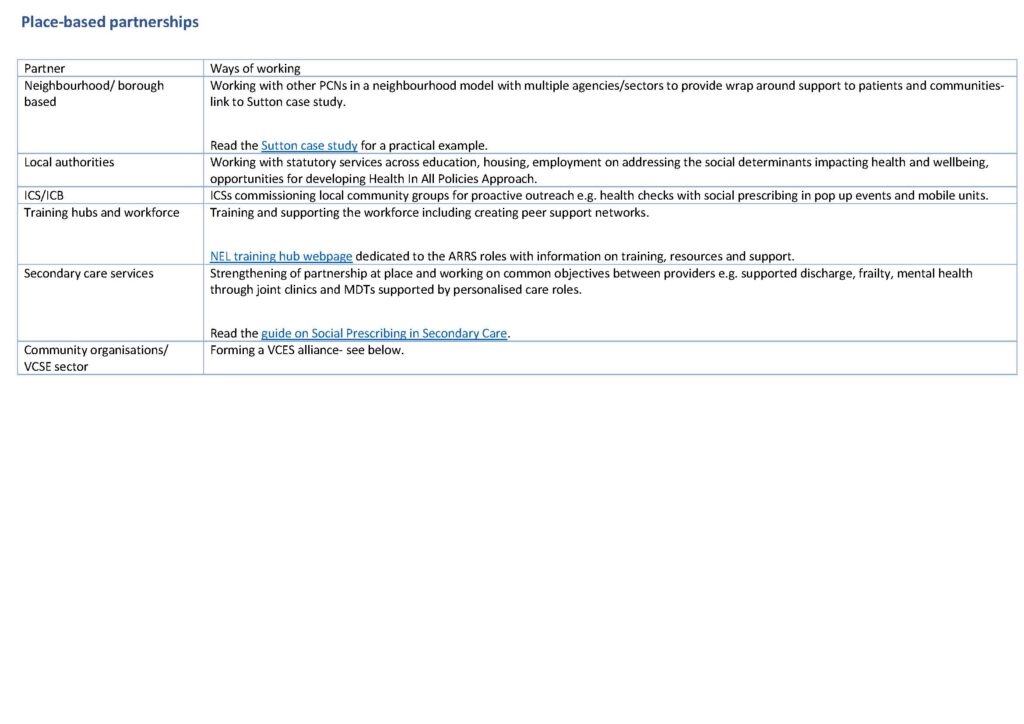
Working in the wider system
Personalised care takes a whole-system approach, integrating care services around the person, across the life course, encompassing physical and mental health and wellbeing, and makes most of the expertise, capacity and potential of people families and communities in delivering better outcomes and experiences. It creates a positive shift in power and decision making that enables people to have more choice, a voice, and improve connection to each other and their communities, representing a new relationship between people, professionals and the health and care system.
A key part of personalisation is using asset-based approaches which highlight the strengths, capacity, knowledge of all those involved.
Individual and community co-benefits of social prescribing and personalised care table
Community approaches
https://www.scdc.org.uk/who/what-is-community-development
https://www.kingsfund.org.uk/publications/communities-and-health
https://www.england.nhs.uk/publication/social-prescribing-and-community-based-support-summary-guide/
Checklist for PCNs to strengthen asset-based partnership working
- Do you have an understanding of the wider determinants of health and how they affect your patients?
- What is your PCN’s purpose and vision around asset-based partnership working?
- Who are your local partners?
– How are your relationships with local partners and broader networks across systems, places and neighbourhoods?
– Which partnerships do you need to develop? (Building existing partnerships or creating new partnerships)
– How do you know which partnerships you need to develop?
- What does a good local partnership working model look like for your PCN? You may want to consider
– What is the context and state of your current relationships/partnerships/ networks?
– What is your scope and purpose?
– How effective and inclusive is your current leadership structure?
– How collaborative and inclusive are your partnerships across sectors/agencies?
– What are your timescales for developing cross-sectoral relationships?
– How do you create conditions to enable different ideas, knowledge, strengths, values and approaches of stakeholders to achieve shared desired goals and outcomes?
– How are local partnerships coordinated and how open and responsive are communication channels?
– How are local partnerships resourced and supported? What opportunities are there for re-orientation and endorsement by the wider system?
– What are the key anchor institutions in your programmes and which providers at place can be strengthened?
– How can a Health In All Policies Approach be fostered? This involves working with local authorities and across levels to consider the health impact of policies generated and opportunities to leverage towards the health system
- How much do participatory approaches feature in strategy and local implementation of interventions? How can these be increased?
This section of the website represents the historical record of a legacy programme which is no longer managed by TPHC, as of mid 2025.